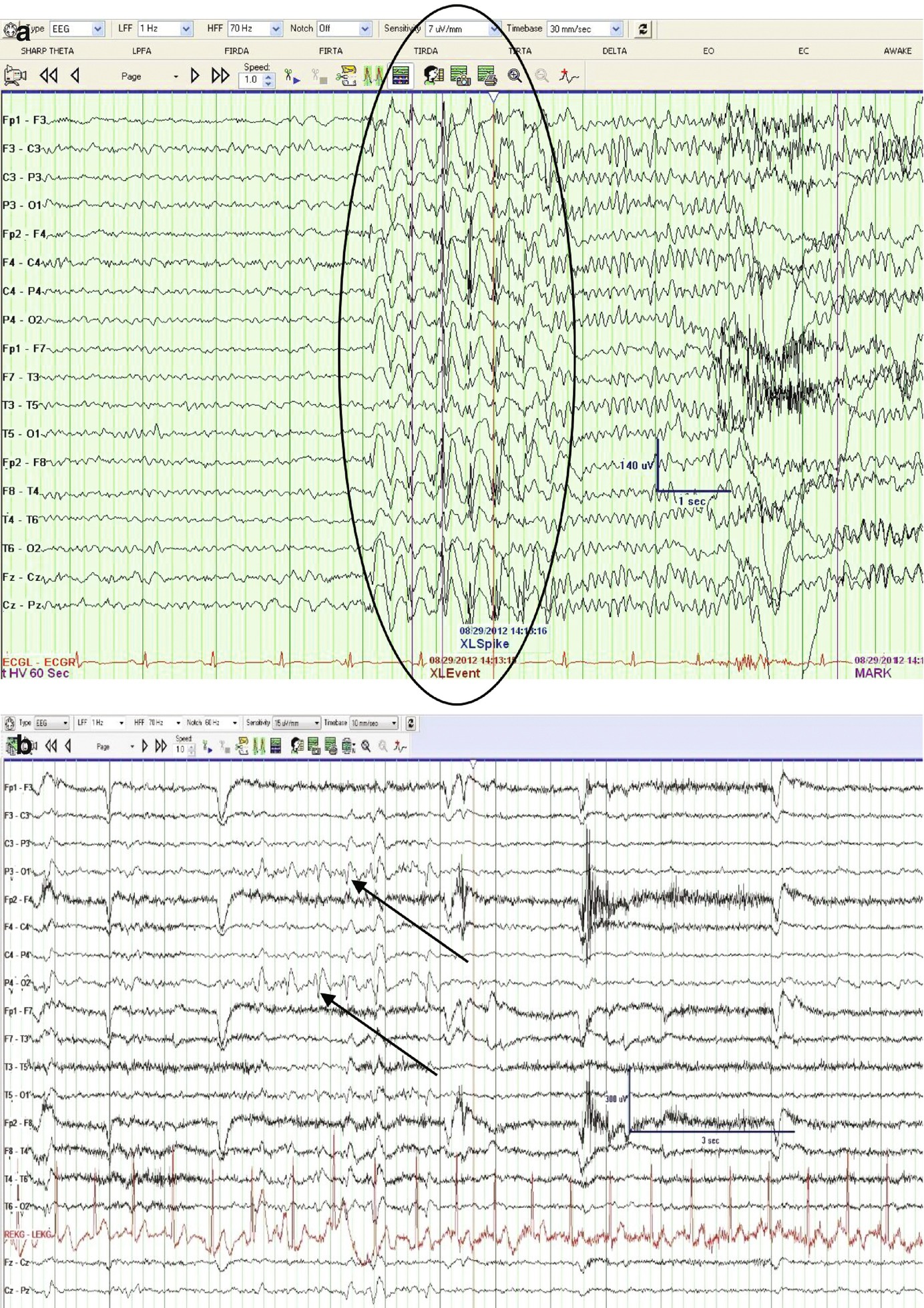
The major differential diagnosis is migraine. Complex illusions are where objects appear disorientated in distance (macroproxiopia, microtelepsia), appear to be distant and minute (teleopsia), appear to have a loss or enhancement of stereoscopic vision, or are persistent or recurrent (palinopsia) (for reviews see Dreifuss, 1985 Sveinbjornsdottir and Duncan, 1993). Lines may appear wavy (dysmorphopsia), objects may appear inclined (plagiopsic) and there may be a loss of colour (achromatopsia). Simple illusions are where objects appear distorted and seem to have changed in size (macropsia or micropsia), shape (metamorphopsia), illumination, colour or clarity. Perceptive illusions may occur, which are classified as simple or complex.
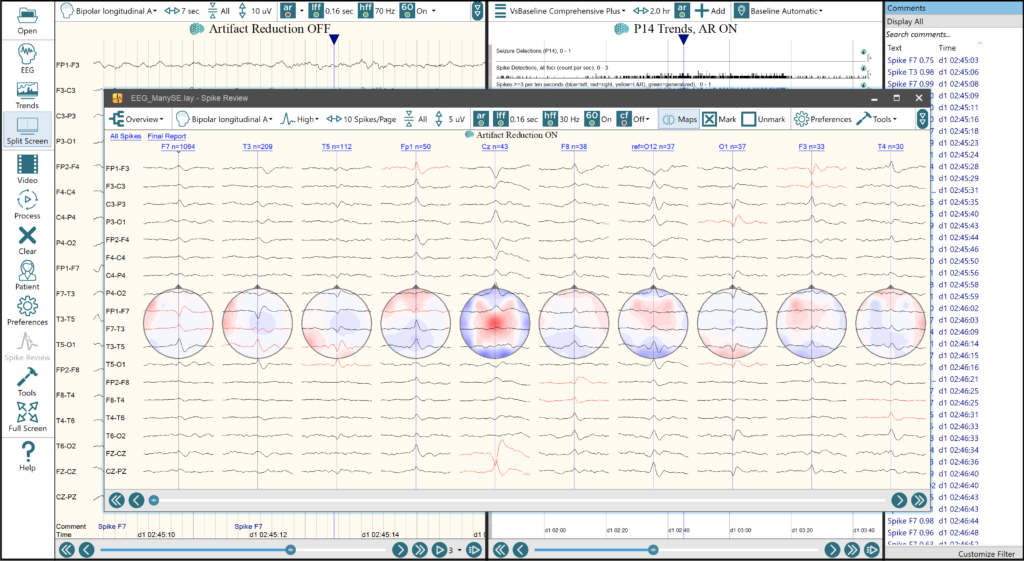
If the occipito‐temporal cortex is involved, the visual hallucinations become complex and colourful, and scenes of varying complexity may be ‘seen’. Positive phenomena are usually flashes of colour or light, which are simple in shape and may be static or mobile. Elementary visual seizures are characterized by fleeting visual manifestations which may be either positive (flashes, phosphenes) or, less commonly, negative (scotoma, hemianopia, amaurosis). Hallucinations typically commence in the visual field contralateral to the affected visual cortex and then spread to involve the entire visual field. Visual hallucinations are the hallmark of occipital seizures, but are not invariably present. Electroclinical features of occipital seizures Additionally we briefly discuss the complexities of the idiopathic occipital epilepsies, including the inter‐relationships between the currently defined syndromes and the idiopathic generalized epilepsies.

Here we highlight the clues to recognition of occipital epilepsies, and discuss a systematic approach to patients emphasizing some of the specific and newly recognized occipital syndromes. As occipital epilepsies are able to emulate other epilepsy syndromes and are a challenge to identify, they may remain undiagnosed. In population studies of newly diagnosed epilepsy, occipital seizures were diagnosed in 1.2–2.6% of cases ( Manford et al., 1992 Jallon et al., 2001). Occipital epilepsy, although relatively uncommon ( Loiseau et al., 1991 Manford et al., 1992 Berg et al., 1999 Jallon et al., 2001), is probably under‐recognized. Emerging evidence suggests that some syndromes have a good surgical outcome, and the consequences to visual function may be less severe than anticipated.Ībbreviations: MELAS = mitochondrial myopathy, encephalopathy, lactic acidosis, and stroke like episodes MERRF = myoclonus epilepsy ragged‐red fibre PME = progressive myoclonus epilepsies PVH = periventricular heterotopia SBH = subcortical band heterotopia Introduction Where medical therapy is ineffective, occipital corticectomy should be considered. We emphasize the clues to recognition of specific occipital epilepsies, some of which now have specific treatments. The idiopathic occipital epilepsies now comprise three identifiable electroclinical syndromes of childhood and adolescence, the biological inter‐relationships and overlap with idiopathic generalized epilepsies of which are discussed here. Major groups include malformations of cortical development, vascular (including epilepsy with bilateral occipital calcifications often associated with coeliac disease), metabolic and the emerging idiopathic occipital epilepsies.

Clinical and neuroimaging advances have led to the recognition of many new occipital epilepsy syndromes, which generally present in childhood or adolescence. When visual symptoms are not prominent, the seizure semiology and scalp EEG may lead the clinician away from considering an occipital focus, as they often reflect seizure propagation rather than seizure origin. Visual hallucinations are the key clinical symptoms indicating an occipital focus, but may be difficult to elicit on history, especially from children, and are not always present. Occipital epilepsies often elude diagnosis as they frequently masquerade as other seizure syndromes.
